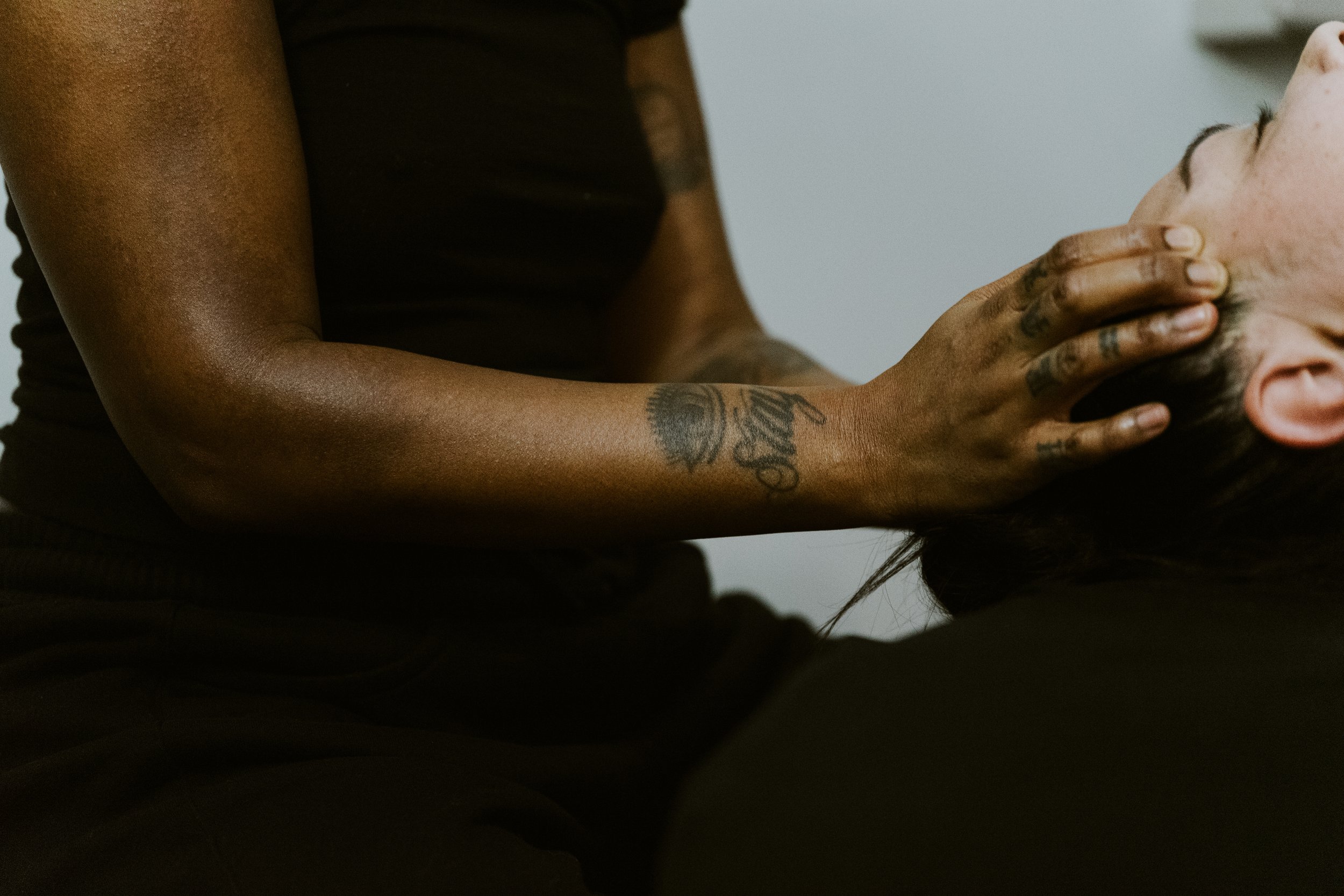What Helps Headaches? Integrative Perspectives
Do you get headaches? If so, you are not alone. While for some they are rare or merely inconvenient, just about everyone knows the unique agony of a headache. Headaches are among the most common of chronic conditions and causes of disability worldwide, affecting around 40% of the world population according to the WHO. Some headaches can be symptoms of more severe, even life-threatening issues. But many headaches are simply headaches–painful, all-consuming, life-disrupting headaches.
As we’ve discussed before, integrative health is not about “either/or”: conventional medicine or complementary and alternative medicine. Headaches are a perfect example of how integrative health can bring together the best of biomedicaland holistic health practices for optimal, whole-person care.
Biomedical Perspectives on Headaches
Did you know that the latest International Classification of Headache Disorders (ICHD-3) identifies over 250 different types of headaches? So many headaches!
According to the Mayo Clinic, headaches can be classified into two major categories: primary and secondary. Primary headaches are a condition unto themselves, while secondary headaches are symptoms resulting from another underlying condition or disease process. (A third category of headaches, relating to neuropathy and facial pain, can be considered as well.)
Primary or Secondary Headaches?
Why does it matter whether a headache is primary or secondary? It’s all about getting the right treatment. This is why Said Isayed says assessment is an important part of a Headache Rescue treatment at MN Integrative Health Studio. Headaches can be symptoms of stroke, meningitis, high blood pressure, and other life-threatening conditions that require immediate intervention. It’s important to be aware of when to seek emergency care for a headache (e.g. stroke, high blood pressure, meningitis), as well as when headaches warrant a visit to the doctor.
“If people never had [a headache] like that before, or it's very severe and came all of a sudden, you should always go to a doctor. There could be possible medication side effects, you need to look into that, or a concussion. It depends. You’ve got to look for red flags and things that need to be referred out. Sometimes you gotta go to the ER. There's a lot of things you can do for a headache, and then there's some things that need more urgent attention.”
Mayo Clinic: When to see a doctor for headaches
Common primary headaches
In biomedical terms, common primary headache diagnoses include tension headaches, migraines, and cluster headaches. Within these categories is an array of human experiences. Our newest practitioner, Yanna Demkiewicz, CMT, notes “there is a wide and prismatic spectrum of the symptoms and causes of headaches and migraines. Headaches and migraines can be caused by dehydration, stress, hormonal changes, lack of sleep, injury, etc., with migraines involving more complex causes i.e. triggers, like light, sound and smell.”
Derrick Lundberg CMT speaks to the underlying physiology uniting headaches, explaining, “pain is such a common symptom that people come in with, but what causes pain in the body? It can be simplified down to pressure on pain sensitive structures called nociceptors."
What makes migraines different from other headaches?
Yanna did research on migraines as part of her studies. Yanna discovered that migraines are one of the oldest known diseases, “with the term first used by the Greek physician and philosopher Galen in the second century AD. Its etymology stems from the Greek word ‘hemicrania,’ which means ‘pain on one side of the head.’ Migraine sufferers know, however, that symptoms are more far-ranging than unilateral head pain; other symptoms include aura, vertigo, tinnitus, exhaustion, brain fog, numbness and tingling in the face and head, and neck pain, with pain symptoms often described as ‘throbbing’ or ‘pulsating’."
MIHS co-owner and Traditional Chinese Medicine (TCM) practitioner Said Isayed, TCMD says in his experience, there may be confusion about what constitutes a migraine. He feels that from a TCM perspective, the differences between patterns of migraine and other types of headaches are significant enough for migraines to warrant a whole separate article. Stay tuned!
Conventional Treatments for Headaches
Biomedical treatments for headaches include over-the-counter and prescription medications. However, lifestyle modifications and non-pharmacological interventions like biofeedback, relaxation techniques, cognitive behavioral therapy, and massage are also recommended. This is in part because while medications can provide important relief, they carry their own risks. In fact, medication overuse headaches itself is a type of headache! Medication overuse headaches can present a risk in the treatment of recurrent headaches, including migraines.
While many people think nothing of popping an over the counter pain pill for a headache, The most common types of over the counter medications have serious adverse effects when used long term, overburdening the organs. A significant number of hospital visits per year are attributable to overuse of ibuprofen, for example. Risks of medication overuse is just one of many reasons to look to the wisdom of Traditional Chinese Medicine when considering headaches.
TCM Perspectives on Headaches
Traditional Chinese Medicine approaches headaches in a fundamentally different way than biomedicine.
MIHS co-owner Larissa Vados PhD, LAc explains:
“Headaches were one of the first examples given to me in how different TCM is in looking at the body vs allopathic medicine. There are only a few types of headaches most commonly diagnosed in allopathic medicine, for example: tension headaches, migraine, and cluster headaches. However, when looking at patients through the TCM lens, two patients presenting with the same diagnosis of tension headache could have completely different diagnoses in TCM, and therefore may also have a completely different treatment strategy from a TCM perspective. While one condition is perceived to be the same between different patients in Western medicine, they can be vastly different according to TCM.”
Ultimately, Said says, to understand headaches, we have to understand the essential needs of the brain: blood flow, or blood qi. From lack of nutrients, to muscle tension, to shallow breathing from emotional stress, to dehydration, to digestive issues, to medication side effects, there are myriad ways that blood flow to the brain can be compromised, resulting in headaches.
TCM Diagnosis: External and Internal, Excess and Deficiency
Said explains that in Chinese Medicine, headaches can be diagnosed as originating either externally or internally. Within these categories, myriad other factors are assessed according to the cosmology of TCM. Among considerations are excess and deficiency, the TCM organ systems (which expand beyond biomedical concepts of their respective organs), the elements, and qi.
External Headaches
Sources of external headaches might include cold, wind, dampness, or other factors coming from outside of the body. Cold wind headaches, for example, are typically associated with tension and pain in the back.
Said says for cold wind headaches, warming the body is essential. “A good tea to make is scallion, ginger, cane, sugar, and tea.”
Dampness headaches are associated with cold humidity, and may be experienced as pressure, heaviness, congestion, and phlegm. Treating the dampness itself is essential to relief from dampness headaches. External headaches tend to be acute and shorter in duration.
Internal Headaches
Internal headaches, says Said, are more likely to be chronic. Internal headaches result from systemic patterns of imbalance. While the headaches may come and go, the subtle underlying issues are persistent. Said says internal headaches may be related to diet, emotions, or what is known in TCM as “deficiency” patterns.
A common internal headache pattern involves the TCM diagnosis of Liver Qi Rising, which is often accompanied by frustration and anger. Oftentimes with Liver Qi Rising headaches, says Said, “people feel like they’re gonna explode.” In TCM worldview, headaches are more prevalent in springtime because Liver is the organ associated with spring. To prevent headaches and support the body in the springtime, Said recommends hydration, movement, and learning from the rhythms of nature. “See what grows in the spring. One of the first things to grow, dandelion, is really good for the liver.”
Excess and Deficiency
Derrick Lundberg CMT holds a Master’s Degree in Acupuncture and Chinese Medicine as well as being a seasoned Integrative Myofascial Release practitioner. Derrick says, “I love the TCM perspective when we are looking to help our patients with their symptoms: TCM has a whole 8 different patterns we associate with headaches, and are generally split into two main categories: excess and deficiency. Excess headaches can feel very intense, and come on quickly; deficiency headaches tend to be more persistent and can be more dull/achy in comparison.”
Said describes a range of deficiency patterns that might result in headaches. Qi blood deficiency can result from overexertion, presenting itself as dull headaches, fatigue, heart palpitation, anemia. Phlegm headaches “are usually related to overeating, sugars, and carbs, which would cause the body to hold a lot of inflammation, and that will restrict blood flow.” He also describes lifestyle related tension headaches, “sitting, driving, computers, phones, causing tension in the neck, or a tight upper back. The pressure could press on nerve endings or could restrict blood flow to the head, which can cause headaches.”
Headache Rescue TCM treatment
In late 2024, MN Integrative Health Studio created a new TCM offering: Headache Rescue Treatment. Headache Rescue was created, Said says, because headaches are such a common reason people come in for treatment: “a lot of people come in for bodywork or Chinese medicine, but their main issue is they have a headache today, something they cannot get relief for.”
Headache Rescue starts with a basic TCM assessment of the whole person in addition to the headache: sleep, digestion, hydration, tongue, pulse, body temperature, and more. What are the underlying patterns that might be causing and contributing to the headache?
Larissa says that Headache Rescue is a great option if you are currently experiencing a headache, or if you suffer from chronic or frequent headaches that are related to muscle tension. “In this treatment we utilize several TCM-based bodywork modalities to help relax muscles in the head, face, neck, and upper body. Treatment may include tuina, gua sha and/or cupping on the back as well as gua sha and/or tuina on the head, face, neck and chest. This is a deeply relaxing treatment that can release muscle tension in the upper body.”
Said adds that these appointments can also include teaching patients at-home exercises to improve posture and interrupt tension-holding patterns. Larissa says that while acupressure (needle-free pressure on acupuncture points) may be used on more distal points including on the upper and lower limbs, acupuncture needles are not typically used in a Headache Rescue Treatment.
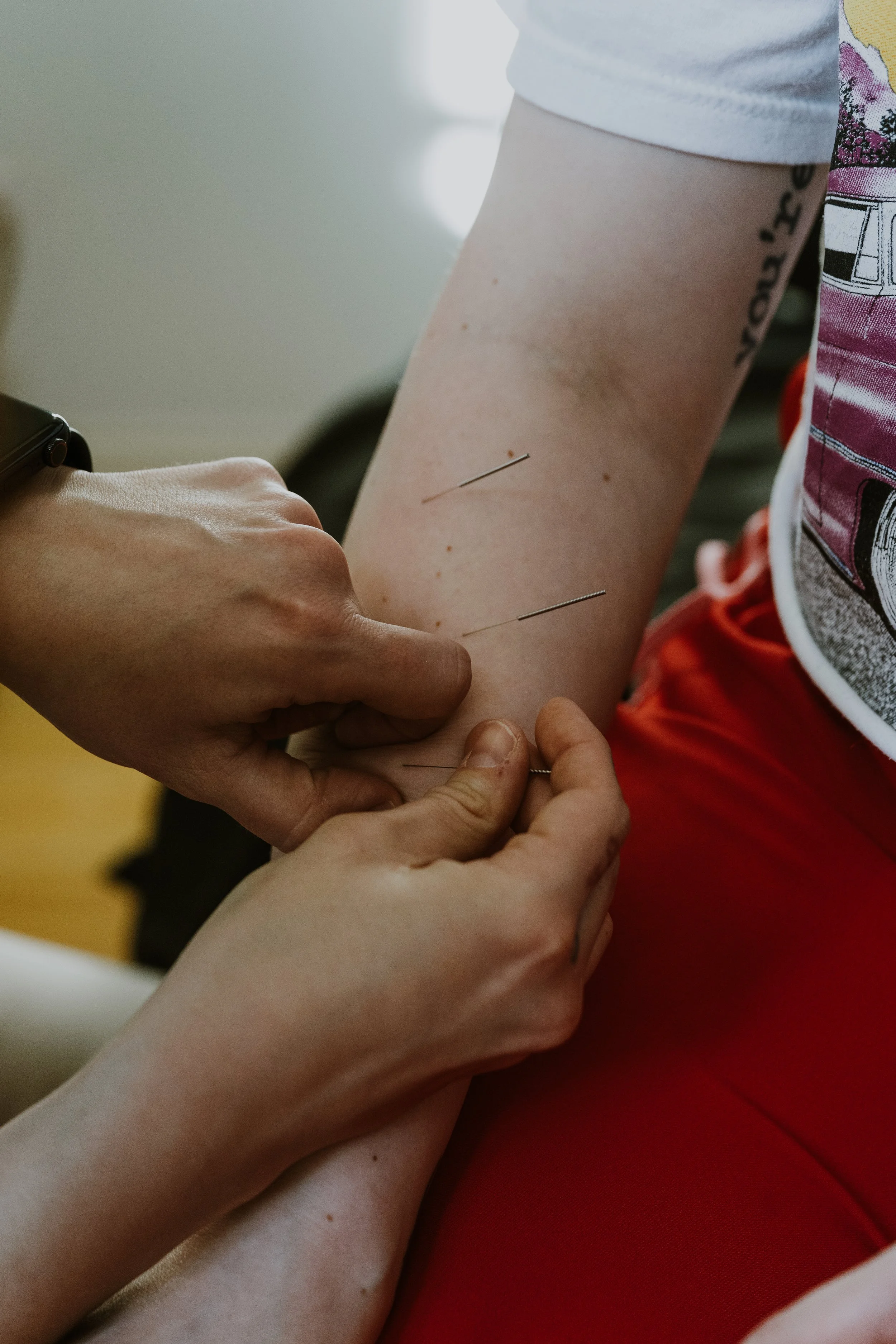
Acupuncture and Headaches
When muscle tension is the main factor in headache patterns, says Larissa, or bodywork is not providing enough relief, an acupuncture appointment may be preferable, explaining:
“Acupuncture has a profound effect on the nervous system, including the brain. Acupuncture can increase and regulate circulation in the brain, stimulate the nervous system to release pain-reducing and anti-inflammatory chemicals, calm over-active nerves in the head and face, and help the nervous system become less sensitive to pain signals.”
You might imagine acupuncture for headaches involving needles on the head…and sometimes this is the case. “For some patients, acupuncture directly in the scalp, head, and neck are very helpful in reducing headache pain,” says Larissa. For others however, “acupuncture points in other areas of the body can be more effective.” Because acupuncture works along meridians that extend throughout the body, “oftentimes in acupuncture appointments we may actually focus more on the distal points in other areas of your body vs points directly on the head or face. There are many acupuncture points on both upper and lower limbs that can be very helpful in reducing headache pain.”
The difference? As always in TCM, the treatment is individualized to the patient.
Learn more about TCM for headaches here.
Other Integrative Approaches to Headaches
Myofascial Release, Neural Manipulation, and Craniosacral Therapy
Derrick agrees that for either excess or deficiency headaches, “acupuncture and especially Traditional Herbal Formulas are an amazing option,” stating that herbal formulas “are a great way to drain away other pathogens, or renourish the tissues so that they are not like a dry sponge shrinking down and compressing on the nociceptors.”
However, Derrick says that in his experience:
“When things are in excess, especially blood stasis, marked by fixed pains and often a stabbing nature, myofascial release is the optimal choice: blood stasis is common when we have a history of injury to the head or neck, concussions, etc. These represent areas where the cranial tissues are stuck and adhered to one another, so there isn't the free flow of fluids and contents within the space available. The fascia being the substrate of the body, then twists around these old injuries, and the pressure in the cranial vault can feel like a rag being wrung out-- 24 hours a day, 7 days a week. It may not always be above a noticeable threshold, but when things get stressful, dehydration sets in, or any number of things which can be the straw that broke the camel’s back. With a fascial modality like acupuncture, Myofascial Release, Neural manipulation, and craniosacral therapy, we can take the wring out of the system and take the pressure off of the nociceptors.”
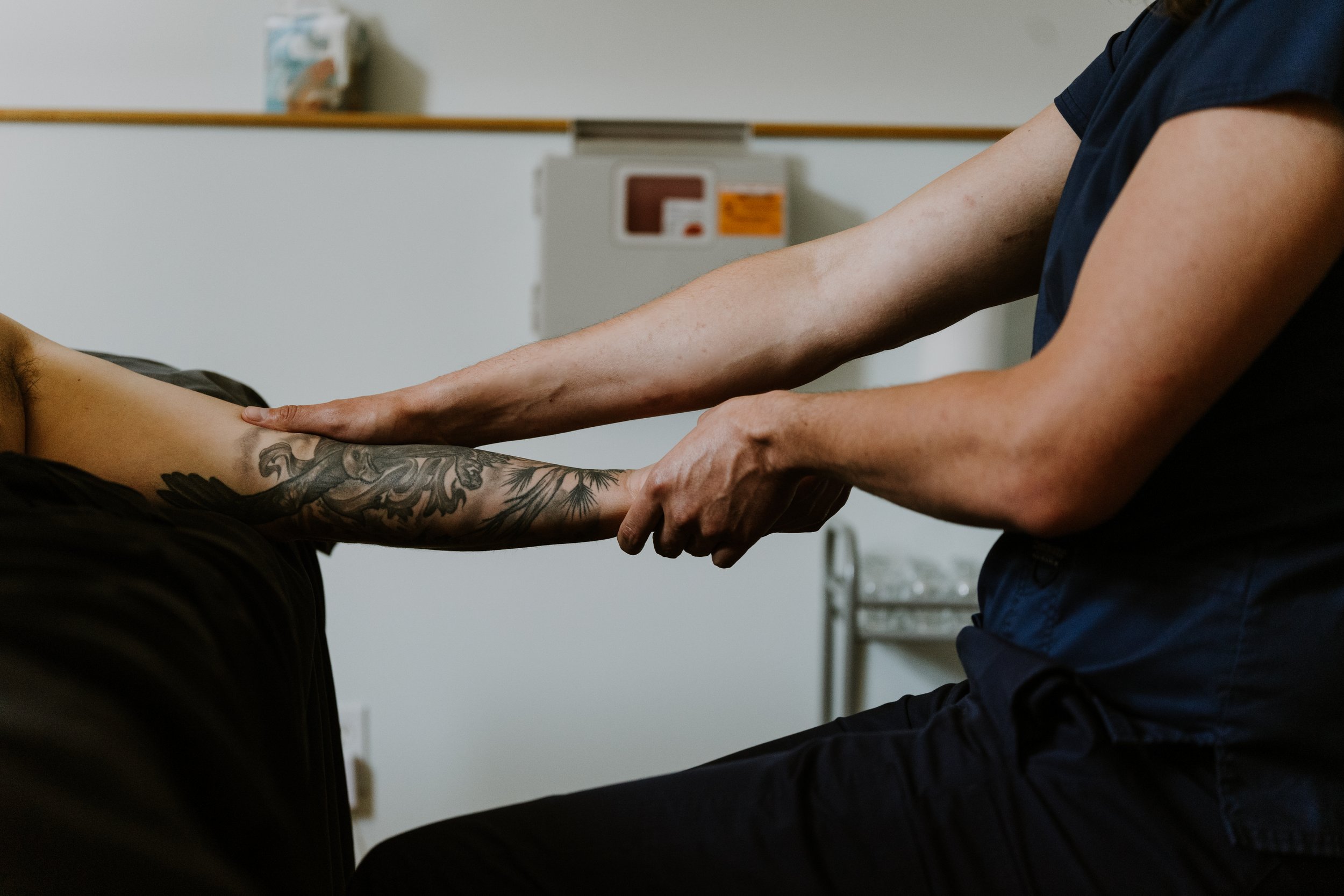
Bodywork for Headaches
Yanna points to the stress-relieving benefits of massage as important for headache relief:
"One aspect of headaches/migraines that massage therapy can support is decreasing stress by activating the parasympathetic nervous system. Stress can trigger both occasional headaches and frequent migraines, and receiving regular massages (weekly, biweekly or monthly, depending on your needs) can support overall wellness and nervous system regulation. Connective tissue massage, Swedish relaxation massage, energy work, safe touch—almost every element and technique of bodywork will reduce stress.”
As for migraines specifically, Yanna says, “There needs to be more research into the impact of massage therapy on migraine patients' symptoms and quality of life—one 2023 study, which only included sixteen women, concludes that patients receiving connective tissue massage treatments on the back and occipital region three times a week for four weeks decreased "pain frequency, duration, intensity, accompanying symptoms, medication use and disability" and increased quality of life; these are positive results, but it's worth noting the small sample size.”
Relaxation Practices for Headaches: Mindfulness, Yoga, Reiki, and other practices
Conventional medicine and TCM find common ground when it comes to stress management as an important lifestyle factor. For many headache patterns, relaxation practices can support relief and prevention. In addition to TCM, acupuncture, and various types of bodywork, practices such as mindfulness, yoga, Reiki, and others that promote the relaxation response may support the body’s needs for optimal balance.
How can we help you with headaches? To find out more about Minnesota Integrative Health Studio services, check out our website. You can book online here. Questions? Feel free to contact us, call (612.345.5648), at or stop by “the studio” on our corner of northeast Minneapolis.
https://www.who.int/news-room/fact-sheets/detail/headache-disorders
https://www.mayoclinic.org/symptoms/headache/basics/causes/sym-20050800
https://www.ninds.nih.gov/health-information/disorders/headache
https://www.mayoclinic.org/symptoms/headache/basics/when-to-see-doctor/sym-20050800
https://www.sciencedirect.com/science/chapter/handbook/abs/pii/B9780128233566000020
Nikolenko VN, Shelomentseva EM, Tsvetkova MM, Abdeeva EI, Giller DB, Babayeva JV, Achkasov EE, Gavryushova LV, Sinelnikov MY. Nociceptors: Their Role in Body's Defenses, Tissue Specific Variations and Anatomical Update. J Pain Res. 2022 Apr 1;15:867-877. doi: 10.2147/JPR.S348324. PMID: 35392632; PMCID: PMC8982820.https://pmc.ncbi.nlm.nih.gov/articles/PMC8982820/
https://www.ninds.nih.gov/health-information/disorders/headache
https://ichd-3.org/8-headache-attributed-to-a-substance-or-its-withdrawal/
https://health.clevelandclinic.org/is-it-bad-to-take-ibuprofen-every-day
Borer JS, Simon LS. Cardiovascular and gastrointestinal effects of COX-2 inhibitors and NSAIDs: achieving a balance. Arthritis Res Ther. 2005;7 Suppl 4(Suppl 4):S14-22. doi: 10.1186/ar1794. Epub 2005 Sep 15. PMID: 16168077; PMCID: PMC2833977.https://pmc.ncbi.nlm.nih.gov/articles/PMC2833977/
McCrae JC, Morrison EE, MacIntyre IM, Dear JW, Webb DJ. Long-term adverse effects of paracetamol - a review. Br J Clin Pharmacol. 2018 Oct;84(10):2218-2230. doi: 10.1111/bcp.13656. Epub 2018 Jul 20. PMID: 29863746; PMCID: PMC6138494.https://pmc.ncbi.nlm.nih.gov/articles/PMC6138494/
Howard RL, Avery AJ, Slavenburg S, Royal S, Pipe G, Lucassen P, Pirmohamed M. Which drugs cause preventable admissions to hospital? A systematic review. Br J Clin Pharmacol. 2007 Feb;63(2):136-47. doi: 10.1111/j.1365-2125.2006.02698.x. Epub 2006 Jun 26. PMID: 16803468; PMCID: PMC2000562.https://pubmed.ncbi.nlm.nih.gov/16803468/
Hao X, Liang F, Wang L, Greenwood KM, Xue CC, Zheng Z, Li Y. Identifying Chinese Medicine Patterns of Tension-Type Headache and Understanding Its Subgroups. Evid Based Complement Alternat Med. 2021 Sep 23;2021:5544571. doi: 10.1155/2021/5544571. PMID: 34603470; PMCID: PMC8483907.https://pmc.ncbi.nlm.nih.gov/articles/PMC8483907/
https://www.mnintegrative.com/blog/spring
Chen Q, Wang M, Fu F, Nie L, Miao Q, Zhao L, Liu L, Li B. Mechanism of Traditional Chinese Medicine in Treating Migraine: A Comprehensive Review. J Pain Res. 2024 Sep 17;17:3031-3046. doi: 10.2147/JPR.S479575. PMID: 39308997; PMCID: PMC11416110. https://pmc.ncbi.nlm.nih.gov/articles/PMC11416110/
Blog from American Migraine Foundation
Headaches - Maciocia https://giovanni-maciocia.com/wp-content/uploads/2021/09/headaches.pdf
Identifying Chinese Medicine Patterns of Tension-Type Headache and Understanding Its Subgroups
https://pmc.ncbi.nlm.nih.gov/articles/PMC8483907/
Integrative East–West Medicine Intervention for Chronic Daily Headache: A Case Report and Care Perspective
Toprak Celenay, Seyda. (2023). An investigation of the effects of connective tissue massage in women with migraine: A controlled clinical trial. Journal of Bodywork and Movement Therapies, Vol. 33. 112-119. https://doi.org/10.1016/j.jbmt.2022.09.008
Faghihi, Zakiyeah. (2025). Massage Therapy by Trained Family Members in Management of Headache in Patients with Migraine: A Double Blinded Randomized Controlled Trial. Jundishapur Journal of Chronic Disease Care, Vol. 14, Issue 2. https://doi.org/10.5812/jjcdc-153468
Öntürk Akyüz, Hatice. (2024). The Effect of Aromatherapy Massage on the Pain Severity and Quality of Life in Acute Migraine Attacks: A Randomized Controlled Trial. Florence Nightingale Journal of Nursing, Vol. 32, Issue 2. DOI: 10.5152/FNJN.2024.23235
Licina E, Radojicic A, Jeremic M, Tomic A, Mijajlovic M. Non-Pharmacological Treatment of Primary Headaches-A Focused Review. Brain Sci. 2023 Oct 8;13(10):1432. doi: 10.3390/brainsci13101432. PMID: 37891800; PMCID: PMC10605615.https://pmc.ncbi.nlm.nih.gov/articles/PMC10605615/
Sic A, Bogicevic M, Brezic N, Nemr C, Knezevic NN. Chronic Stress and Headaches: The Role of the HPA Axis and Autonomic Nervous System. Biomedicines. 2025 Feb 13;13(2):463. doi: 10.3390/biomedicines13020463. PMID: 40002876; PMCID: PMC11852498.https://pmc.ncbi.nlm.nih.gov/articles/PMC11852498/#sec8-biomedicines-13-00463
Kachhadia MP, Khalil ZM, Shah S, Fawad M, Sajjad H, Yadav KP, Kanthala NR, Patel T, Egbujo UC, K B. Role of Yoga as Adjunctive Therapy for Migraines: A Narrative Review of the Literature. Cureus. 2023 Nov 7;15(11):e48434. doi: 10.7759/cureus.48434. PMID: 38073999; PMCID: PMC10701189.https://pmc.ncbi.nlm.nih.gov/articles/PMC10701189/#sec3